Q fever osteomyelitis is a zoonotic infection prevalent worldwide caused by the bacteria Coxiella burnetii, a fastidious obligate intracellular microorganism. It can survive in the external environment for long periods in a spore-like state and may be carried long distances by wind.1–4 Cattle, sheep, and goats are commonly infected; human transmission happens mainly by breathing the contaminated dust, exposure to body fluids of infected animals, or by ingestion of contaminated dairy products.3,4 Most cases are reported in spring and early summer, coinciding with the peak of birthing season for cattle, sheep, and goats.
Although Q fever is reported to be endemic in the Middle East, the disease remains underdiagnosed, particularly in children, because of the wide range of its clinical presentations. In 2003, a report from Oman showed that in a sample of 54 healthy goats, 28 (52%) were infected with C. burnetii.5 More recently, a study of 1193 camels in 278 randomly selected herds in Oman revealed a mean seroprevalence of 19.4% (individual level range: 1.4–32.5%; herd level range: 5.4–52.4%), suggesting coxiellosis to be endemic in Omani camels.6
Most human infections of C. burnetii are asymptomatic. About 40% of cases show wide-ranging clinical signs such as acute flu-like illness, hepatitis, pneumonia, and rarely, endocarditis.7 The disease can become chronic in 1–2% of patients.7,8 Studies have shown that people with heart valve defects, endocarditis, or heart valve implants may have higher risk of chronic infection and severe disease. Although pediatric Q fever is mostly self-limiting, in rare cases it can follow a course of relapsing febrile illness lasting several months or even years.7
The first clinical case of Q fever in Oman was reported in 1997 with presentation of chronic pericarditis while the second case (1999) presented with acute pneumonia.9 Both patients were adults. The first pediatric chronic Q fever endocarditis case was reported in 2019 in a child with congenital heart disease who was treated successfully with antibiotics.10 A study conducted in 2001 on the seroprevalence in 102 adults from northern Oman revealed that 9.8% were seropositive from previous C. burnetii infections.5
We describe the first confirmed case of chronic osteomyelitis caused by C. burnetii infection in an Omani child who had contact with domestic animals.
Case Report
A previously healthy four-year-old Omani girl from Masirah Island (located off the east coast of mainland Oman), presented with a six-week history of mild pain and subsequent swelling in her left ankle following trauma after a fall while playing in her home garden. Her parents took her to a local health center and private clinics. Despite antibiotic courses, the swelling did not resolve. On 7 July 2019, the child was admitted in Khoula Hospital, Muscat, a major trauma and orthopedic hospital in Oman. Magnetic resonance imaging (MRI) showed osteomyelitis of the left talus bone. An orthopedic surgeon and a radiologist reviewed the MRI and confirmed the presence of a cavitary lesion on the left talus with surrounding edema and periosteal collection, suggesting osteomyelitis [Figure 1]. On admission, the child underwent debridement and drainage of her lesion. Intra-operational findings showed clinical evidence of osteomyelitis of left talus bone with cavitary lesion with pus and granulation tissue, samples of which were sent for microbiological and histopathological testing.
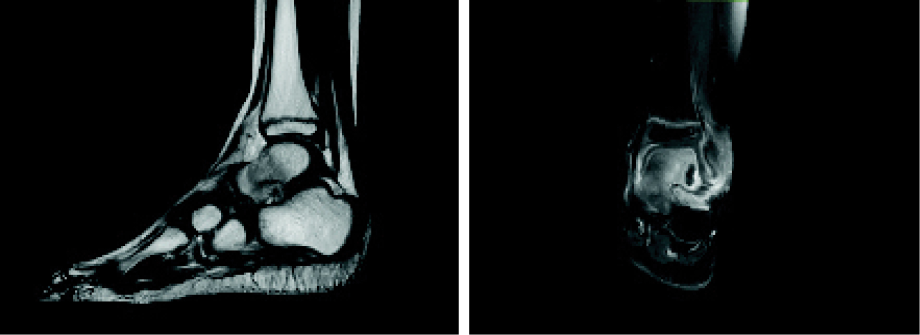 Figure 1: Magnetic resonance imaging of the left foot at presentation showing talus cavitary lesion with periosteal collection.
Figure 1: Magnetic resonance imaging of the left foot at presentation showing talus cavitary lesion with periosteal collection.
Postoperatively, the child was started on cloxacillin intravenously, under the assumption that the most likely cause of osteomyelitis at her age was methicillin-sensitive Staphylococcus aureus. She remained hemodynamically stable and afebrile. The baseline blood workup revealed a normal white blood cell count of 7.3 × 103/µL, absolute neutrophil count of 3.3 × 103/µL, platelets 353 × 103/µL, and C reactive protein < 1 mg/L. Tests for renal function, liver function, and coagulation yielded normal results. Blood cultures (three bottles) yielded negative for bacterial growth after prolonged incubation. Bone biopsy and pus samples were also negative for bacterial growth after prolonged incubation of two weeks; gram stain showed a few polymorphonuclear cells but no organisms. The bone and pus samples were further investigated for tuberculosis, Brucella, and Coxiella using polymerase chain reaction (PCR), as the parents gave a history of animal contact and consumption of raw milk. The child’s grandmother kept goats and sheep in a farm beside the house, a few of whom had died shortly after giving birth.
Laboratory investigations for mycobacterial infection on bone and pus specimens included Zeihl-Neelsen stain for acid-fast bacilli, mycobacterial culture, and PCR (Cepheid GenXpert, Xpert MTB/RF). All the tests yielded negative results. Samples were also sent to the Central Public Health Laboratories, Oman, for multiplex zoonotic PCR which tested for three microorganisms: Brucella, C. burnetii, and Streptococcus pneumoniae. Only C. burnetii PCR was positive in both bone and pus samples with a very low cycle threshold values of 22 and 28, respectively. However, a blood sample remained negative for C. burnetii PCR. C. burnetii serology (Virion Serion ELISA classic C. burnetii phase 1 and phase 2 serology) was indicative of chronic infection and were immunoglobulin (Ig) G phase 1 positive and IgA phase 1 positive. The IgG phase 2 was positive, while the IgM phase 2 was negative. Samples were sent to Laboratoire Cerba, Saint-Ouen-l’Aumône, France, for immunofluorescence analysis (IFA) as this gold-standard test was not available locally. IFA results confirmed the diagnosis of chronic C. burnetii infection with a high level of IgG antibodies in both phases 1 and 2. The C. burnetii IgG phase 1 titer was 1:2048 and IgM phase 1 titer was < 1:3200. The C. burnetii IgG phase 2 titer was 1:5120 and the IgM phase 2 of < 1:3200 [Table 1]. Histopathological examination of explanted tissue of pus and bone revealed evidence of granulomas suggestive of chronic infection [Figure 2].
Table 1: Immunofluorescence analysis of serum samples.
|
July 2019
|
1:2048
|
< 1:320
|
1:512
|
< 1:320
|
Ig: immunoglobulin. The analysis was conducted at Laboratoire Cerba, Saint-Ouen-l’Aumône, France.
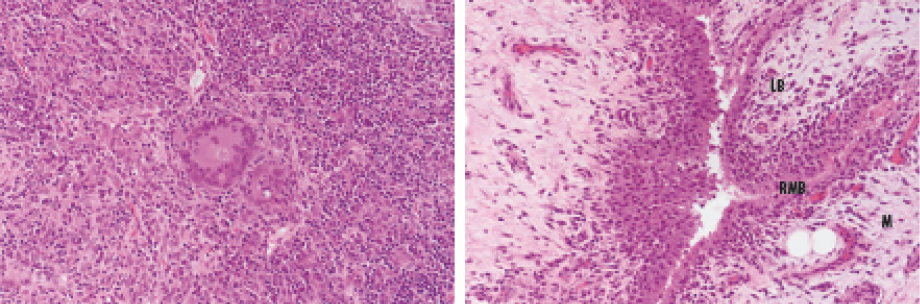 Figure 2: Histopathology sections of the bone tissue biopsy taken intraoperatively (20 × inflamed synovium).
Figure 2: Histopathology sections of the bone tissue biopsy taken intraoperatively (20 × inflamed synovium).
The child remained stable throughout her three-week hospital stay. She was managed by a multidisciplinary team of pediatric infectious disease consultants, microbiologists, and orthopedic surgical consultants. We started her on a combination of three drugs (ciprofloxacin IV, cotrimoxazole IV, and rifampicin oral) targeting C. burnetii. Doxycycline and hydroxychloroquine were avoided due to their safety issues in children. After two weeks she became unable to tolerate oral rifampicin, which was stopped. Ciprofloxacin-cotrimoxazole combination IV was continued for another week and thereafter switched to oral. In three weeks, the swelling subsided and she was able to bear weight on her left foot.
The child was discharged on 31 July 2019. Her parents were counseled on the source and nature of her infection and our long-term management plan. Regular visits to the orthopedic and pediatric infectious disease clinics were scheduled. A repeat IFA three months after treatment initiation showed a 50% reduction in titers [Table 1]. During the follow-up visits the child was doing well and her left foot X-ray suggested a reduction in infection. The child was referred to an immunologist to exclude possible primary and secondary immunodeficiency disorders and no immunological defect was confirmed. Fourteen months after the initiation of the antibiotic combination, the left ankle X-ray showed the lesion as completely resolved [Figure 3]. The clinical and laboratory results were also positive, and the antibiotics were stopped. A follow-up sample for IFA was sent to the same reference laboratory in France and results are awaited. The child continues to do well with scheduled visits to pediatric infectious disease and orthopedic clinics before final discharge.
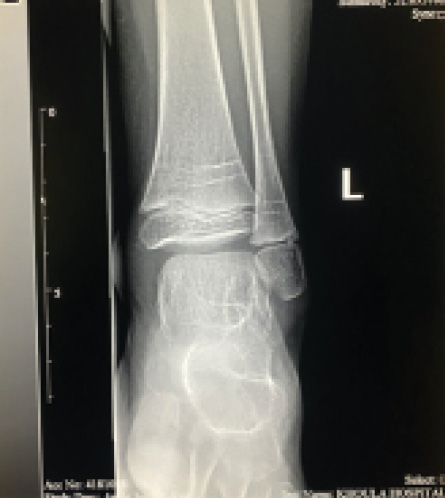 Figure 3: Left ankle X-ray after 14 months of antibiotics course.
Figure 3: Left ankle X-ray after 14 months of antibiotics course.
Discussion
We report the first confirmed case of osteomyelitis due to C. burnetii infection in a previously healthy Omani child. Q fever is a nationally notifiable disease in Oman and is considered an emerging zoonotic infection that remains challenging.11 To ascertain its exact epidemiology in Oman, comprehensive seroprevalence studies are needed. A recent study in Iran using real-time PCR detection of the IS1111 gene confirmed that 4.2% of 216 suspected cases were positive for C. burnetii.12 Comparable prevalence has been reported from East Azerbaijan (3.6%) and Mazandaran province of Northern Iran (5.3%).13 Another Iranian study reported seroprevalence of IgG phase I and II antibodies at 19.80% and 32.86%, respectively.14 Variable levels of seroprevalence have been reported among adult blood donors in Egypt: 20% in the Suez Canal area; 16% in the Nile Valley; and 10% in the Nile Delta.15 Antibodies to C. burnetii were reported in 18.3% of blood donors in Morocco and 26% in Tunisia.16 A tertiary center in Saudi Arabia reported 19 cases of Q fever in the period 2009–2018.17 In the Netherlands, an acute Q fever epidemic comprising 4000 cases occurred from 2007 to 2010, leading to six deaths.18,19
Vaccination is a viable option to control this disease. In Australia a nationally-funded vaccination drive halved that country’s Q fever rates between 2002 and 2006.20 Q fever being endemic in the Middle East, we support the introduction of the vaccine in this region as well.21
As Q fever symptoms can vary widely and mimic other common conditions, most clinicians fail to spot it in their differential diagnosis. Laboratory tests are essential to confirm a clinical diagnosis. These are mainly based on serological tests, qualitative enzyme-linked immunosorbent assay, as well as quantitative IFA, the gold standard.
Aid to diagnosis is provided by the tendency of C. burnetii to manifest in two distinct antigenic variants—a virulent variant ‘phase I’ and an avirulent one ‘phase II’. In acute Q fever, the titer of the antibody against the phase II variant is generally higher than the antibody that targets the phase I variant. Acute disease is mostly diagnosed via a relative increase in the phase II antibody within three to four weeks of the onset of the disease. In chronic cases the phase I antibody dominates. The variations in the titer of antibodies against phases I and II may persist for months or years after the initial infection.8
The modern molecular PCR-based tests allow diagnosis of early acute Q fever. The PCR tests in tissue samples from our patient showed a very high C. burnetii load. Histological examination of tissues showed granuloma formation [Figure 2] providing definitive confirmation of the infection. Further, some children with chronic Q fever may have a specific immunological defect that has been implicated in the delayed clearance of the infection.22 Our patient was investigated and found free of this defect.
Due to the broad variety of clinical presentations of Q fever in children, it remains underdiagnosed; there are but isolated reports of chronic pediatric cases.23 Q fever in children is often asymptomatic with frequently described clinical symptoms as generic as fever with respiratory or gastrointestinal symptoms.24 Severe manifestations such as osteomyelitis have been rarely described.24 Although a combination of doxycycline plus hydroxychloroquine is recommended, we did not adopt it for several reasons including the young age of our patient, the risk of teeth discoloration, and the uncertain long-term effectiveness of this treatment for osteomyelitis. Although our patient did not tolerate oral rifampicin beyond two weeks, it was possible to manage her infection with a combination of oral ciprofloxacin and cotrimoxazole treatment, highlighting the need for further research to evolve clear treatment guidelines for pediatric Q fever.
Conclusion
Q fever osteomyelitis is a relatively rare and underreported disease in Oman. We successfully treated our case with a combination of oral ciprofloxacin and cotrimoxazole, avoiding the doxycycline-hydroxychloroquine combination. Surgical debridement helped establish the diagnosis and had therapeutic value as well. While the course we adopted may be suitable for other pediatric Q fever cases, we suggest more research on Q fever treatment in children and issuance of clear guidelines, particularly regarding the use and safety of doxycycline-hydroxychloroquine combination in pediatric patients.
Disclosure
The authors declared no conflicts of interest. Written consent has been obtained from the patients.
Acknowledgments
We acknowledge the institutions where this case was investigated, managed, and followed up. These include the Royal Hospital’s infection disease department, the Khoula Hospital’s departments of medical microbiology, orthopedics, and radiology, and the Central Public Health Laboratories where the Reverse transcription-PCR testing was conducted.
references
- 1. Maurin M, Raoult D. Q fever. Clin Microbiol Rev 1999 Oct;12(4):518-553.
- 2. Norlander L. Q fever epidemiology and pathogenesis. Microbes Infect 2000 Apr;2(4):417-424.
- 3. Eldin C, Mélenotte C, Mediannikov O, Ghigo E, Million M, Edouard S, et al. From Q fever to Coxiella burnetii infection: a paradigm change. Clin Microbiol Rev 2017 Jan;30(1):115-190.
- 4. Angelakis E, Raoult D. Q fever. Vet Microbiol 2010 Jan;140(3-4):297-309.
- 5. Scrimgeour EM, Al-Ismaily SI, Rolain JM, Al-Dhahry SH, El-Khatim HS, Raoult D. Q fever in human and livestock populations in Oman. Ann N Y Acad Sci 2003 Jun;990:221-225.
- 6. Hussain MH, Al-Makhladi S, Al-Rawahi A, Rajamony S, Al-Zadjali MS, Asubaihi S, et al. Seroprevalence of Coxiella Burnetii (Q Fever) antibodies in the camels (Camelus Dromedarius) of the Sultanate of Oman. Proceedings of the 4th Conference of ISOCARD, Kazakhstan; 2015. 251-252.
- 7. Anderson A, Bijlmer H, Fournier PE, Graves S, Hartzell J, Kersh GJ, et al. Diagnosis and management of Q fever–United States, 2013: recommendations from CDC and the Q fever working group. MMWR Recomm Rep 2013 Mar;62(RR-03):1-30.
- 8. Raoult D, Marrie T, Mege J. Natural history and pathophysiology of Q fever. Lancet Infect Dis 2005 Apr;5(4):219-226.
- 9. Scrimgeour EM, Johnston WJ, Al Dhahry SH, El-Khatim HS, John V, Musa M. First report of Q fever in Oman. Emerg Infect Dis 2000 Jan-Feb;6(1):74-76.
- 10. Al Araimi H, Al-Alawi K, Al-Jardani A, Paul G, Al-Sukaiti N, Al-Farqani A, et al. Chronic Q fever endocarditis in an Omani child: the first pediatric case report from Oman. Oman Medical Journal 2020;35(5):e180.
- 11. Awaidy SA, Al Hashami H. Zoonotic diseases in Oman: successes, challenges and future directions. Vector Borne Zoonotic Dis 2020;20(1):1-9.
- 12. Esmaeili S, Mohabati Mobarez A, Khalili M, Mostafavi E, Moradnejad P. Genetic evidence of Coxiella burnetii infection in acute febrile illnesses in Iran. PLoS Negl Trop Dis 2019 Feb;13(2):e0007181.
- 13. Khalili M, Naderi HR, Salehnia N, Abiri Z. Detection of Coxiella burnetii in acute undifferentiated febrile illnesses (AUFIs) in Iran. Trop Doct 2016 Oct;46(4):221-224.
- 14. Mohabbati Mobarez A, Bagheri Amiri F, Esmaeili S. Seroprevalence of Q fever among human and animal in Iran; A systematic review and meta-analysis. PLoS Negl Trop Dis 2017 Apr;11(4):e0005521.
- 15. Botros BA, Soliman AK, Salib AW, Olson J, Hibbs RG, Williams JC, et al. Coxiella burnetii antibody prevalences among human populations in north-east Africa determined by enzyme immunoassay. J Trop Med Hyg 1995 Jun;98(3):173-178.
- 16. Letaief AO, Yacoub S, Dupont HT, Le Cam C, Ghachem L, Jemni L, et al. Seroepidemiological survey of rickettsial infections among blood donors in central Tunisia. Trans R Soc Trop Med Hyg 1995 May-Jun;89(3):266-268.
- 17. Elzein FE, Alsherbeeni N, Alnajashi K, Alsufyani E, Akhtar MY, Albalawi R, et al. Ten-year experience of Q fever endocarditis in a tertiary cardiac center in Saudi Arabia. Int J Infect Dis 2019;88:21-26.
- 18. van der Hoek W, van de Kassteele J, Bom B, de Bruin A, Dijkstra F, Schimmer B, et al. Smooth incidence maps give valuable insight into Q fever outbreaks in The Netherlands. Geospat Health 2012 Nov;7(1):127-134.
- 19. Roest HI, Tilburg JJ, van der Hoek W, Vellema P, van Zijderveld FG, Klaassen CH, et al. The Q fever epidemic in The Netherlands: history, onset, response and reflection. Epidemiol Infect 2011 Jan;139(1):1-12.
- 20. Gidding HF, Wallace C, Lawrence GL, McIntyre PB. Australia’s national Q fever vaccination program. Vaccine 2009 Mar;27(14):2037-2041.
- 21. Jaff D, Wilson P. Q fever: a neglected disease in the Middle East. J Health Systems 2016;11(2):12-14.
- 22. Nourse C, Allworth A, Jones A, Horvath R, McCormack J, Bartlett J, et al. Three cases of Q fever osteomyelitis in children and a review of the literature. Clin Infect Dis 2004 Oct;39(7):e61-e66.
- 23. Maltezou HC, Raoult D. Q fever in children. Lancet Infect Dis 2002 Nov;2(11):686-691.
- 24. Slok EN, Dijkstra F, de Vries E, Rietveld A, Wong A, Notermans DW, et al. Estimation of acute and chronic Q fever incidence in children during a three-year outbreak in the Netherlands and a comparison with international literature. BMC Res Notes 2015 Dec;8(1):1-7.