Cerebral venous sinus thrombosis (CVST) is a rare cause of stroke, usually affecting young to middle-aged patients.1 It accounts for 0.5–1% of all causes of stroke.1 Despite advances in recognizing this condition, CVST remains a challenging disease because of its variable clinical presentation. There are several risk factors for the development of CVST, which are classified into acquired and genetic factors. Surgery, trauma, pregnancy, puerperium, exogenous hormones, and antiphospholipid syndrome are examples of acquired risk factors, whereas deficiencies in antithrombin, protein C, and protein S are examples of genetic factors2 in addition to bacterial meningitis.3
Headache is the main presenting symptom, which is described as diffuse and often progresses in severity over days or weeks.4 In addition, one-third to three-quarters of cases present with focal deficits such as hemiparesis, hemisensory disturbance, seizures, an impaired level of consciousness, and papilloedema.4 Patients with extensive involvement of the deep cerebral veins can present with coma and pyramidal signs.4 The diagnosis of CVST is typically based on clinical suspicion and imaging. Magnetic resonance imaging (MRI) combined with magnetic resonance venography is the best imaging strategy when computed tomography (CT) of the brain is equivocal for CVST.5 Antithrombotic treatment modalities include heparin, thrombolysis, and oral anticoagulants are used to treat CVST.5 The clinical presentation and outcomes of these patients have not been described in Oman. We, therefore, sought to describe the clinical presentation of CVST and outcomes of patients in Oman.
Methods
We conducted a retrospective cohort study of records from two tertiary care hospitals in Oman, Royal Hospital (RH) and Armed Forces Hospital (AFH), between January 2006 and June 2016. The study was reviewed and approved by the ethics committees of the two hospitals. Patients with a diagnosis of CVST were identified using the hospital medical records with an International Statistical Classification of Diseases version 10 (ICD-10) coding of CVST (cerebral infarction due to cerebral venous thrombosis, nonpyogenic). We included Omani patients, aged 14 years or older (usually cared for by the adult service) with a radiologically confirmed diagnosis of CVST. A search using the ICD-10 returned 81 patients of which 27 were not included (14 were non-Omani, three had no radiological confirmation, and 10 were less than 14 years old). We recorded patients’ demographic data, clinical features, laboratory and radiological investigations, and in-hospital management and outcomes.
All patients underwent basic investigations, such as complete blood count, serum electrolytes, renal and liver function tests, coagulation studies, blood sugar levels, and chest radiographs. Thrombophilia screen, vasculitis workup, and JAK2 mutation analysis were sent for most patients.
Continuous variables were presented as means or medians, while categorical variables were presented as frequency and percentages. Age was compared using the Student t-test. A p-value of < 0.050 was considered statistically significant. SPSS Statistics (IBM Corp. Released 2011. IBM SPSS Statistics for Windows, Version 20.0. Armonk, NY: IBM Corp.) was used to analyze the data.
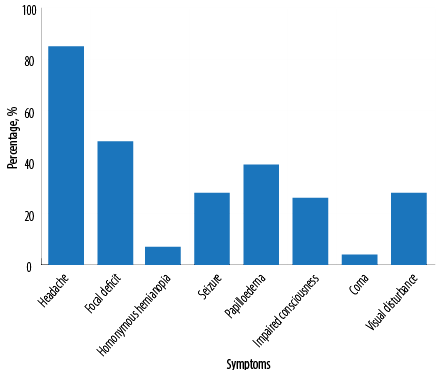
Figure 1: Presenting symptoms of cerebral venous sinus thrombosis.
Results
A total of 54 patients were included from the two centers (RH = 46; AFH = 8) who fulfilled the inclusion criteria. The median age was 32 years (range = 18–78). There were 35 (64.8%) females and 19 (35.2%) males. The median duration of presenting illness was 10 days (range = 1–120) before the diagnosis of CVST. Figure 1 illustrates the frequency of presenting symptoms on admission: headache was the most common (85.0%) followed by focal neurological deficit (48.0%) and seizures (27.0%). One patient had a seizure with status epilepticus at presentation and required intubation and mechanical ventilation. Papilloedema was found in 39.0% of cases while 26.0% presented with an impaired level of consciousness (defined as Glasgow Coma Scale of < 14). Four percent had coma at presentation requiring intubation and mechanical ventilation. Five patients presented with proptosis, chemosis, and external ophthalmoplegia. Multiple sites of CVST were found in 21 patients (38.9%), sigmoid and/or transverse sinus thrombosis in 19 (35.2%) [Figure 2], and sagittal sinus thrombosis in nine (16.7%). The distribution of thrombosis is illustrated in Figure 3.
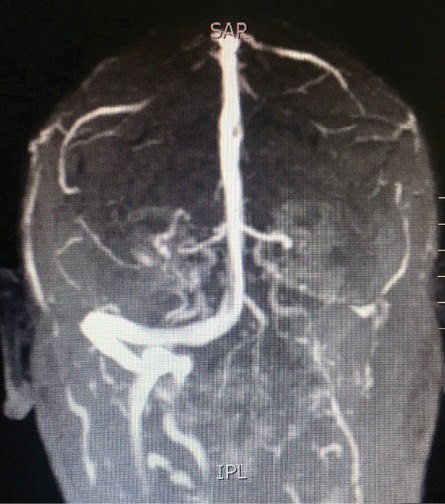
Figure 2: A magnetic resonance imaging of a patient with left transverse sinus thrombosis.
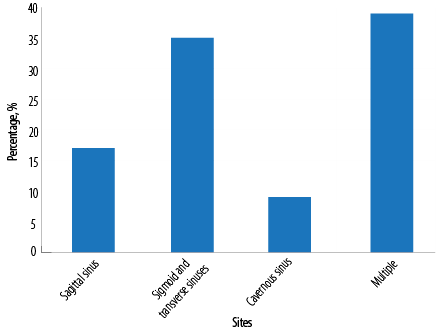
Figure 3: Sites of cerebral venous sinus thrombosis involvement.
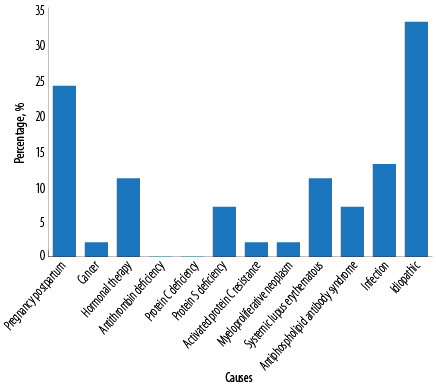
Figure 4: Causes of cerebral venous sinus thrombosis.
Pregnancy and postpartum accounted for 24.0% of all causes of CVST in our cohort [Figure 4]. All pregnant patients presented in the first trimester. All postpartum patients delivered by cesarean section and presented in the first two weeks. Infection was evident in 13.0% of our cohort, of which, two patients had invasive mucormycosis, two had bacterial meningitis, two had periorbital cellulitis, and one had cerebral malaria. All patients received appropriate antimicrobials according to culture and sensitivity. Hormonal therapy accounted for 11.0% of all causes of CVST; six of 35 (17.1%) were using hormonal therapy for primary infertility or birth control. None had a history of smoking or other hormonal disturbances. Eleven percent of patients had systemic lupus erythematous. Antiphospholipid antibody syndrome and inherited thrombophilia accounted for 7.0% and 11.0% of cases, respectively. One patient had adenocarcinoma of the stomach with liver metastasis and another had neurosarcoidosis. No cause was identified in 33.0% of patients. Two patients had hemorrhagic stroke complicating their CVST, and the treating physician opted to continue subcutaneous anticoagulation with unfractionated heparin. None of our cohort developed hemorrhage after initiation of anticoagulation.
Most patients (89.0%) received therapeutic low molecular weight heparin subcutaneously followed by oral anticoagulants. One patient was treated with unfractionated heparin as they had associated cerebral hemorrhage. No patient underwent thrombolysis. Thirty-seven patients (68.5%) were discharged with no neurological sequelae. Sixteen (29.6%) had residual weakness in the form of hemiplegia, monoplegia, or dysphasia at discharge. Younger patients were more likely to be discharged without neurological sequelae. The median age for patients without neurological sequelae was 31 years, which was significantly different than the median age of patients with sequelae (55 years, p = 0.003). Gender and duration of illness were not predictive of the sequelae (p > 0.050). One patient died after discharge at six months follow-up.
Discussion
CSVT presents in a wide variety of signs and symptoms, ranging from isolated headache to focal deficits and impaired level of consciousness. The clinical presentation of our cohort was similar to what has been reported from one of the largest registries for CVST with headache being the most common presenting symptom.2 An impaired level of consciousness accounted for 26.0% of all presenting complains, which was slightly higher than the 22% reported in the International Study on Cerebral Vein and Dural Sinus Thrombosis (ISCVT).2 However, the prevalence of coma was greater in the ISCVT (14%) compared to our study (4.0%).2 The median duration from onset of symptoms to hospital presentation was 10 days compared to four days in the ISCVT study.2
Pregnancy and the postpartum period accounted for 24.0% of all female cases presenting with CVST in our study. This is in comparison to the ISCVT, which showed that pregnancy accounted for 6.3% of cases.2 Eleven percent of females presented within two weeks postpartum compared to 13.8% in the ISCVT. A possible explanation for these differences is that the birth rates in our countries are higher than that in the west and we might encounter more cases either during pregnancy or in the postpartum period. We noted that hormone use accounted for 11.0% of CVST cases compared to 58.6% in the ISCVT, which may be a reflection of the limited use of hormonal therapy in Oman.2
Inherited thrombophilia, which is an important cause of CVST, is higher in western countries2 (22.4% vs. 11.0% in Oman). This could explain the relatively small number of cases in our study. However, our figure is similar to that reported in neighboring countries like Saudi Arabia (12.5%).6 The majority of patients (89.0%) in our study received anticoagulation therapy, which is similar to the number given in the ISCVT (85%).2
Our mortality rate at discharge and six months follow-up was 0.0 and 1.9%, respectively, compared to 4.3% and 6.8%, respectively, in the ISCVT study.2 We noted that 29.8% had residual weakness at discharge compared to 12.6% in the ISCVT,2 and age was an important predictor of this unfavorable outcome. A recent study published from Oman representing a major tertiary care academic center included 30 patients diagnosed with CVST based on CT and/or MRI.7 Most patients (83%) presented with headache, which was similar to our study. They had a higher rate of seizure (40%) compared to our study. All patients were started on low molecular weight heparin and 77% of patients recovered with no sequelae compared to 89.0% in our study.
Our study was limited by its retrospective design and small sample size. Moreover, there were no uniform evaluation in terms of workup for thrombophilia and autoimmune disorders. Our study has several strengths. This is the first study reporting CVST in Omani patients and illustrating differences reported in the literature. The information from this study and another recently published from another major tertiary center in Oman7 can be used as baseline data for planning future clinical care and research for this group of patients.
Conclusion
Pregnancy and postpartum were the most common predisposing factors for CVST in our cohort. Although the mortality rate is low, the risk of residual neurological deficit remains high. We recommend a prospective study for better characterization and outcome assessment.
Disclosure
The authors declared no conflicts of interest. No funding was received for this study.
references
- 1. Saposnik G, Barinagarrementeria F, Brown RD Jr, Bushnell CD, Cucchiara B, Cushman M, et al; American Heart Association Stroke Council and the Council on Epidemiology and Prevention. Diagnosis and management of cerebral venous thrombosis: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2011 Apr;42(4):1158-1192.
- 2. Ferro JM, Canhão P, Stam J, Bousser MG, Barinagarrementeria F, Investigators I; ISCVT Investigators. Prognosis of cerebral vein and dural sinus thrombosis: results of the International Study on Cerebral Vein and Dural Sinus Thrombosis (ISCVT). Stroke 2004 Mar;35(3):664-670.
- 3. Hemasian H, Hakamifard A. Thrombophilic evaluation in cases of cerebral venous sinus thrombosis. Oman Med J 2018 Nov;33(6):537.
- 4. Allroggen H, Abbott RJ. Cerebral venous sinus thrombosis. Postgrad Med J 2000 Jan;76(891):12-15.
- 5. Issar P, Chinna S, Issar SK. Evaluation of cerebral venous thrombosis by CT, MRI and MR venography. J Assoc Physicians India 2017 Nov;65(11):16-21.
- 6. Khealani BA, Wasay M, Saadah M, Sultana E, Mustafa S, Khan FS, et al. Cerebral venous thrombosis: a descriptive multicenter study of patients in Pakistan and Middle East. Stroke 2008 Oct;39(10):2707-2711.
- 7. Lal D, Gujjar AR, Ramachandiran N, Obaidi A, Kumar S, El-Tigani M, et al. Spectrum of cerebral venous thrombosis in Oman. Sultan Qaboos Univ Med J 2018 Aug;18(3):e329-e337.