Scrub typhus is a potentially fatal rickettsial infection. Usually, it presents as acute febrile illness, and multiorgan involvement can be seen.1 The disease is caused by Orientia tsutsugamushi, an obligate intracellular Gram-negative bacterium, and is transmitted by infected chigger larva. This mite-borne disease is distributed from Asia to the Pacific islands from Pakistan to Northern Australia, Japan, Korea, China, and Thailand and causes substantial mortality. This region is known as the Tsutsugamushi Triangle.2 In Nepal, scrub typhus is an emerging neglected tropical disease.3 This article reports the first case of scrub typhus imported to Oman.
Case report
In late August 2017, a previously healthy 28-year-old male was admitted with an acute febrile illness. He had a four-day history of rigors, headache, anorexia, and maculopapular skin rash. He arrived from Nepal three days before the start of his symptoms. At the initial assessment, he appeared well, alert, and conscious. His body temperature was 40 °C, and he had marked conjunctival injection as well as a diffuse maculopapular rash. A black crusted skin lesion was present on his left upper arm [Figure 1]. Initial laboratory test results are shown in Table 1. Empirical therapy with ceftriaxone 2 g was started. Malaria, dengue fever, Crimean-Congo hemorrhagic fever, leptospirosis, brucellosis, and Q fever were excluded by microscopy, serology or molecular tests as well as Epstein-Barr virus, cytomegalovirus, HIV, hepatitis B, and hepatitis C infections. At the same time, repeated blood and urine cultures remained negative.
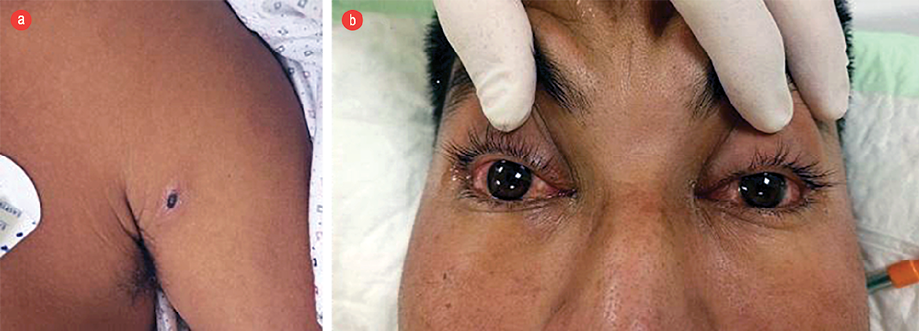
Figure 1: (a) Typical eschar seen on the patient’s arm. (b) Conjunctival injection.
Table 1: Laboratory test results during hospitalization.
|
ALT |
0–40 U\L |
47 |
NT |
212 |
199 |
141 |
NT |
|
Hematocrit |
35–45% |
53 |
43 |
37 |
35 |
44 |
33 |
|
Platelets |
140–400 × 109/L |
91 |
40 |
38 |
48 |
135 |
190 |
|
WBC |
4.0–11.0 × 109/L |
3.8 |
2.0 |
5.2 |
8.8 |
11.0 |
5.5 |
|
Neutrophils |
2.5–7.5 × 109/L |
3.2 |
1.5 |
4.7 |
7.5 |
7.9 |
2.8 |
|
Lymphocytes |
1.5–3.5 × 109/L |
0.5 |
0.5 |
0.3 |
0.5 |
2.6 |
1.8 |
ALT: alanine aminotransferase; WBC: white blood cells; CRP: C-reactive protein; NT: not tested.
On the ninth day of illness, he became tachycardic (102 beats/min) and tachypneic (30 breaths/min), his blood pressure decreased to 95/60 mmHg, and he developed chest crepitations bilaterally. A chest X-ray showed features suggestive of acute respiratory distress syndrome (ARDS) and cardiomegaly. Echocardiography showed mild pericardial effusion with borderline right ventricular dysfunction. He became unconscious, and his Glasgow coma scale score was 7. Brain computed tomography showed massive brain edema. Empirical antibiotic treatment was continued with piperacillin/tazobactam (PTZ) 4.5 g every eight hours and clarithromycin 500 mg every 12 hours, and the brain edema was treated with mannitol and dexamethasone. Gradually, he started to improve and was extubated. After three days of intravenous PTZ and clarithromycin, treatment was continued with oral doxycycline 100 mg every 12 hours as the good response to macrolide therapy, patients’ clinical presentation, laboratory results, and epidemiological data implied that the patient had a rickettsial infection. After seven days of oral therapy, he was discharged in an excellent condition 15 days after admission. A positive Weil-Felix agglutination test (taken after discharge) indicated that the patient most probably had scrub typhus.
Weil-Felix agglutination testing of the patient’s pretreatment serum sample was positive for OXK antigen with an antibody titer of 1200 (Remel Europe Ltd, UK). As this test is neither specific nor sensitive additional tests of the pretreatment and convalescent serum sample taken three weeks later were done in the Naval Medical Research Center, Silver Spring, USA. The Orientia tsutsugamushi immunofluorescence assay (IFA) slides (Biocell Diagnostics, USA) were used for IFA as recommended by the manufacturer. Enzyme-linked immunosorbent assay (ELISA) was performed as previously described by Chao and coworkers.4 Both the IFA and ELISA tests showed more than four-fold antibody titer increase between the admission and the convalescence serum sample confirming that the patient had scrub typhus.
Discussion
Our patient presented with an acute febrile illness and a rash, so the differential diagnosis had to include various diseases.5,6 Characteristic skin eschar in an acute febrile patient from the Tsutsugamushi Triangle is a valuable sign in scrub typhus diagnosis. The frequency of eschars in patients with scrub typhus is highly variable and can be seen in 11–44% of patients.7,8
Scrub typhus complications can be manifested by ARDS, encephalitis, interstitial pneumonia, acute renal and/or hepatic failure as well as acute myocarditis. Respiratory system involvement during scrub typhus ranges from 20–70% out of which ARDS is seen in 14% patients.9,10 Cardiomegaly is found in 3.5% of patients with scrub typhus.11,12 Mortality can reach 70% in untreated patients. It varies according to location and increases with age as well as severe disease-related complications like myocarditis, delirium, pneumonitis, or signs
of hemorrhage.13,14
Conclusion
The patient presented here is the first reported and confirmed case of scrub typhus in Oman. The disease was imported to Oman as the patient had recently returned from Nepal. Many people travel to Oman from the Tsutsugamushi Triangle so scrub typhus should be kept in mind as early treatment can prevent mortality.
Disclosure
The authors declared no conflicts of interest.
references
- 1. Varghese GM, Trowbridge P, Janardhanan J, Thomas K, Peter JV, Mathews P, et al. Clinical profile and improving mortality trend of scrub typhus in South India. Int J Infect Dis 2014 Jun;23:39-43.
- 2. Bonell A, Lubell Y, Newton PN, Crump JA, Paris DH. Estimating the burden of scrub typhus: a systematic review. PLoS Negl Trop Dis 2017 Sep;11(9):e0005838.
- 3. Upadhyaya BP, Shakya G, Adhikari S, Rijal N, Acharya J, Maharjan L, et al. Scrub typhus: an emerging neglected tropical disease in Nepal. J Nepal Health Res Counc 2016 May;14(33):122-127.
- 4. Chao CC, Zhang Z, Belinskaya T, Thipmontree W, Tantibhedyangkul W, Silpasakorn S, et al. An ELISA assay using a combination of recombinant proteins from multiple strains of Orientia tsutsugamushi offers an accurate diagnosis for scrub typhus. BMC Infect Dis 2017 Jun;17(1):413.
- 5. Sivarajan S, Shivalli S, Bhuyan D, Mawlong M, Barman R. Clinical and paraclinical profile, and predictors of outcome in 90 cases of scrub typhus, Meghalaya, India. Infect Dis Poverty 2016 Oct;5(1):91.
- 6. Koraluru M, Nandigam M, Bairy I, Vidyasagar S, Varma M. Multiple eschars in scrub typhus: a case report. Trop Doct 2017 Jan;47(1):67-69.
- 7. Wi YM, Woo HI, Park D, Lee KH, Kang CI, Chung DR, et al. Severe fever with thrombocytopenia syndrome in patients suspected of having scrub typhus. Emerg Infect Dis 2016 Nov;22(11):1992-1995.
- 8. Takhar RP, Bunkar ML, Arya S, Mirdha N, Mohd A. Scrub typhus: a prospective, observational study during an outbreak in Rajasthan, India. Natl Med J India 2017 Mar-Apr;30(2):69-72.
- 9. Abhilash K, Mannam PR, Rajendran K, John RA, Ramasami P. Chest radiographic manifestations of scrub typhus. J Postgrad Med 2016 Oct-Dec;62(4):235-238.
- 10. Wang CC, Liu SF, Liu JW, Chung YH, Su MC, Lin MC. Acute respiratory distress syndrome in scrub typhus. Am J Trop Med Hyg 2007 Jun;76(6):1148-1152.
- 13. Song SW, Kim KT, Ku YM, Park SH, Kim YS, Lee DG, et al. Clinical role of interstitial pneumonia in patients with scrub typhus: a possible marker of disease severity. J Korean Med Sci 2004 Oct;19(5):668-673.
- 14. Charoensak A, Chawalparit O, Suttinont C, Niwattayakul K, Losuwanaluk K, Silpasakorn S, et al. Scrub typhus: chest radiographic and clinical findings in 130 Thai patients. J Med Assoc Thai 2006 May;89(5):600-607.
- 11. Bithu R, Kanodia V, Maheshwari RK. Possibility of scrub typhus in fever of unknown origin (FUO) cases: an experience from Rajasthan. Indian J Med Microbiol 2014 Oct-Dec;32(4):387-390.
- 12. Taylor AJ, Paris DH, Newton PN. A systematic review of mortality from untreated scrub typhus (Orientia tsutsugamushi). PLoS Negl Trop Dis 2015 Aug;9(8):e0003971.