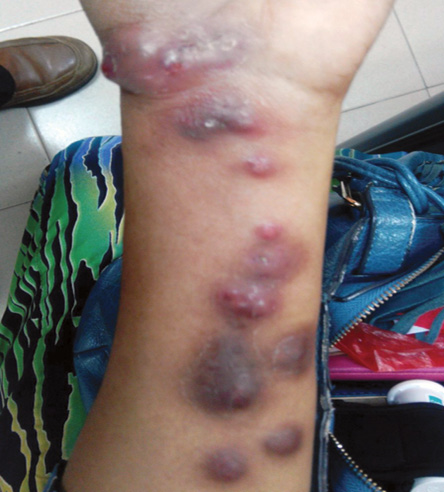
Figure 1: Erythematous, non-tender nodules, and papules, some with central crusting distributed over the ventral aspect of the left wrist and forearm.
A 50-year-old woman with an underlying type 2 diabetes mellitus presented with a three-month history of multiple non-tender nodules over the ventral aspect of her forearm [Figure 1]. The nodules appeared after she was scratched by a domestic cat, which was later euthanized for an undiagnosed cutaneous disease. She was otherwise well with no other constitutional symptoms. Examination revealed multiple well-demarcated non-fluctuant nodular lesions in her left wrist extending to the forearm with varying sizes. Some of the lesions appeared to be erythematous while others were hyperpigmented. The remainder of systemic physical examinations was unremarkable.
Questions
- What is the most likely diagnosis?
a. Cutaneous tuberculosis.
b. Erythema nodosum.
c. Leishmaniasis.
d. Leprosy.
e. Sporotricosis.
- What are the differential diagnoses?
a. Bacterial pyoderma.
b. Inflammatory dermatophyte infections.
c. Primary cutaneous nocardiosis.
d. Leishmaniasis.
e. Blastomycosis.
f. Chromoblastomycosis.
g. Cutaneous tuberculosis.
h. All of the above.
- What investigation is indicated?
a. Mantoux test.
b. Skin slit smear.
c. Fine needle aspiration cytology.
d. Punch biopsy.
- What is the management?
a. Start antituberculosis treatment.
b. Start clofazamine treatment.
c. Start itraconazole treatment.
d. Start topical paromomycin treatment.
Answers
- e. Sporotrichosis (lymphocutaneous).
- h. All of the above.
- d. Punch biopsy for direct examination and culture.
- c. Itraconazole, terbinafine, or potassium iodide.
Discussion
Sporotrichosis is a subacute to chronic fungal infection caused by the dimorphic fungi Sporothrix schenckii.1–3 It is mainly associated with occupational disease and usually caused by minor cuts during soil or plant handling. However, on rare occasions it can also be a zoonotic infection transmitted by an infected feline.2 Sporotrichosis is widely distributed worldwide and commonly occurs in adults < 30 years old; however, pediatric sporotrichosis has been documented.2,3
Sporotrichosis infections mainly involve cutaneous or subcutaneous infection and lymphatics. Lymphocutaneous infection is the most common presentation followed by a fixed type. Disseminated and extracutaneous manifestation involving pulmonary and osteoarticular infection usually occur in immunocompromised patients such as those with human immunodeficiency virus infection and acquired immune deficiency syndrome (HIV/AIDS).3
Lymphocutaneous sporotrichosis causes skin lesions with characteristic proximal nodular lymphangitic spread.4–6 The characteristic skin lesion pattern in patients with a history of trauma (during typical occupational exposure) are highly suggestive of sporotrichosis.5,6 The primary skin lesion, which develops one to 12 weeks after fungal inoculation usually ulcerates and is followed by proximal nodular lesions across the lymphatic channels. This is typically described as the ‘sporotrichoid’ characteristic spread. Patients are typically asymptomatic, and routine laboratory testing is normal.
Sporotrichosis can be mistaken for many skin infections such as bacterial pyoderma, inflammatory dermatophyte infection, nocardiosis, leishmaniasis, blastomycosis, chromoblastomycosis, and cutaneous tuberculosis.3,7 As cutaneous nocardiosis, cutaneous nontuberculous mycobacterial infections, and cutaneous leishmaniasis may present with similar skin manifestation, the diagnosis of sporotrichosis needs to be established by culture and/or histopathological demonstration of the fungus from aspiration or biopsy of skin lesions.
The gold standard for a definitive diagnosis of sporotrichosis is fungal culture. Material aspirated or swabbed from a skin lesion or sample from a tissue biopsy should be inoculated onto Sabouraud’s dextrose agar and incubated at room temperature for four weeks.8 Histopathological examination reveals a mixed pyogenic and granulomatous inflammation with occasional asteroid bodies, which consist of a central basophilic yeasts surrounded by eosinophilic material (Splendore-Hoeppli phenomenon). However, histopathological examination has a lower sensitivity compared to fungal culture.5,6 Occasionally, a yeast form of Sporothrix schenkii can be seen in biopsy samples. Both microbiological and histopathological examinations of skin lesions are also important to rule out other infections that manifest with ‘sporotrichoid’ skin lesion patterns.9 Serological antibody measurement is also available, but is costly.4
Treatment with antifungal drugs is the mainstay for sporotrichosis.4–7Azole groups are the drugs of choice for this infection. The recommended treatment is itraconazole 200 mg per day for three to six months.3,7 Terbinafine has also been recommended as treatment for sporotrichosis but is more expensive.7 Alternatively, saturated solution of potassium iodide (SSKI), which has been used historically for the treatment of sporotrichosis is still being used as a mainstay treatment in low-income countries with inaccessibility to other drugs. Even though SSKI is cheap, it is inconvenient to administer and may cause problems with tolerability due to its frequent adverse effects. Fluconazole and ketoconazole should only be used if the above agents could not be tolerated due to its relatively lower response rate.10 Prognosis is excellent with clinical improvement typically observed within four weeks of therapy initiation.
references
- 1. Yegneswaran PP, Sripathi H, Bairy I, Lonikar V, Rao R, Prabhu S. Zoonotic sporotrichosis of lymphocutaneous type in a man acquired from a domesticated feline source: report of a first case in southern Karnataka, India. Int J Dermatol 2009 Nov;48(11):1198-1200.
- 2. Bhutia PY, Gurung S, Yegneswaran PP, Pradhan J, Pradhan U, Peggy T, et al. A case series and review of sporotrichosis in Sikkim. J Infect Dev Ctries 2011 Aug;5(8):603-608.
- 3. Nelson IA. Spirothricosis. In: Medscape Drug and disease [cited 2016 March]. Available from: http://emedicine.medscape.com/article/228723-overview.
- 4. Barros MB, de Almeida Paes R, Schubach AO. Sporothrix schenckii and Sporotrichosis. Clin Microbiol Rev 2011 Oct;24(4):633-654.
- 5. Rex JH, Okhuysen PC. Sporothrix schenckii. In Mandell GL, Bennett JE, Dolin R, editors. Principles and practice of infectious diseases. 6th ed. Philadelphia, PA: Churchill Livingstone; 2005:2984-2987.
- 6. Kauffman CA. Sporotrichosis. Clin Infect Dis 1999 Aug;29(2):231-236, quiz 237.
- 7. Coskun B, Saral Y, Akpolat N, Ataseven A, Ciçek D. Sporotrichosis successfully treated with terbinafine and potassium iodide: case report and review of the literature. Mycopathologia 2004 Jul;158(1):53-56.
- 8. Pappas PG, Tellez I, Deep AE, Nolasco D, Holgado W, Bustamante B. Sporotrichosis in Peru: description of an area of hyperendemicity. Clin Infect Dis 2000 Jan;30(1):65-70.
- 9. Kostman JR, DiNubile MJ. Nodular lymphangitis: a distinctive but often unrecognized syndrome. Ann Intern Med 1993 Jun;118(11):883-888.
- 10. Kauffman CA, Pappas PG, McKinsey DS, Greenfield RA, Perfect JR, Cloud GA, et al. Treatment of lymphocutaneous and visceral sporotrichosis with fluconazole. Clin Infect Dis 1996 Jan;22(1):46-50.