Anterior cruciate ligament (ACL) injury is one of the most common and debilitating sports-related knee injuries in young, active populations, and it frequently requires surgical reconstruction to restore joint stability and function.1 Although extrinsic factors—such as playing surface, footwear, and sport-specific demands—contribute to risk of injury, recent research has highlighted the role of intrinsic anatomical factors.2 Among these, femoral intercondylar notch morphology, particularly its width and anatomical shape, has emerged as an important determinant in ACL injury risk,3 shifting the scientific focus from external mechanisms to the structural environment “inside the notch”.
The femoral intercondylar notch is a groove located at the distal femur that accommodates the cruciate ligaments and the meniscofemoral ligaments.4 Van Eck et al,5 described an arthroscopic classification of notch morphology into A-shaped, U-shaped and W-shaped variants. In that study, A-shaped notch was the most prevalent. Height was also shown to influence notch shape, with taller patients more likely to have U- or W-shaped notches. Furthermore, A-shaped notch was associated with up to 73% increased risk of ACL tear, while U- and W-shaped notches were linked to lower risks (approximately 32.5%).3,5 Subsequently, studies from different parts of the world examined angular notch parameters, particularly the transverse notch angle (TNA) and sagittal notch angle (SNA), as potential markers of ACL pathology. A decreased TNA and an increased SNA, frequently observed in narrower A-shaped notches, are associated with degeneration of ACL [Figure 1].5–8
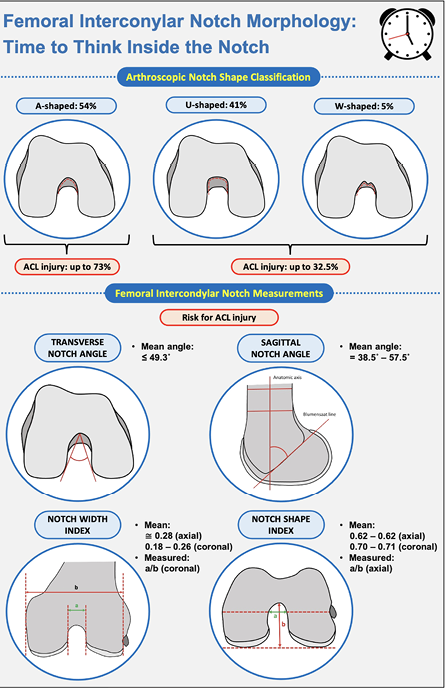 Figure 1: Femoral intercondylar notch morphology as a potential risk factor for anterior cruciate ligament injury.
Figure 1: Femoral intercondylar notch morphology as a potential risk factor for anterior cruciate ligament injury.
Kim et al,6 in Korea, recognized the association of a decreased TNA (≤ 47.4°) and the presence of mucoid degeneration. Similarly, Raja et al,7 found significantly decreased intercondylar notch angle (mean 49.3°) in axial plane among Indian patients with ACL injuries. In Spain, Alentorn-Geli et al,8 also found that ACL-injured patients had a significantly narrower TNA of 46.5°, compared with 50.7° in controls. Regarding the SNA, Fernandez-Jaen et al,9 of Spain reported notable differences between individuals with intact and torn ACLs, with mean angles of 56.2° and 57.5°, respectively.9 In Poland, Bouras et al,10 observed a slightly greater SNA in ACL-injured patients (44°) compared to controls (43°). In contrast, Huang et al,11 of China reported a smaller SNA in patients with ACL injury (38.5°) than in controls without ACL injury (41.1°), based on sagittal magnetic resonance imaging (MRI) measurements.11 Thus, despite using similar measurement techniques, these studies demonstrated inconsistent results, indicating that SNA is not a reliable indicator of ACL injury. Therefore, further studies are needed to clarify the clinical relevance of SNA in the context of ACL injuries.
There have been a large number of investigations on notch width index (NWI) and notch shape index (NSI) as potential risk factors for ACL injury, using both radiographic and MRI modalities.3,6–8 The literature reports that a smaller NWI is associated with an increased risk of sustaining an ACL injury.3 Kim et al,6 observed that a smaller NWI of 0.271 was significantly associated with mucoid degeneration of the ACL on MRI. Raja et al,7 found an NWI of 0.272 in patients with ACL injures, compared to 0.285 in the control group. They also reported smaller NSI values in ACL-injured patients: 0.624 in the axial plane and 0.700 in the coronal plane, compared to 0.661 and 0.709, respectively, in the control group.
In Poland, Ficek et al,10 evaluated the NWI and NSI on axial and coronal MRI in patients with cyclops syndrome after ACL reconstruction (ACLr), ACL-injured patients, and controls. Both indices were lower in ACL-injured and cyclops-ACLr patients than in controls, suggesting that intercondylar notch geometry may increase the risk of ACL injury and cyclops lesion formation.10 In contrast, a Spanish study by Alentorn-Geli et al,8 found no significant association between NWI and ACL injury, showing the uncertainty of the predictive value of this parameter.
Today, it is increasingly important to “think inside the notch”. Variations in the shape of the femoral intercondylar notch have been associated with an increased risk of ACL injury across diverse populations. These anatomical differences can influence intraoperative decision-making during ACLr, particularly with regard to intercondylar notch morphology. In this context, selective notchplasty may play a critical role in protecting the ACL graft and reducing the risk of reinjury during the postoperative healing phase.
references
- 1. Voskuilen R, Dietvorst M, van der Steen M, Janssen RP. A small notch width index, steeper medial and lateral tibial slope and higher lateral/medial tibial slope ratio are relevant knee morphological factors for ACL injuries in skeletally immature patients-A systematic review. J Exp Orthop 2025 Mar;12(1):e70211.
- 2. Apseloff NA, Hughes JD, Devitt BM, Musahl V. Primary anterior cruciate ligament injury: extrinsic and intrinsic risk factors. J Am Acad Orthop Surg 2024 Sep;33(13):693-702.
- 3. Andrale R, Vasta S, Sevinas N, Pereira R, Leal A, Papalia R, et al. Notch morphology is a risk factor for ACL injury: a systematic review and meta-analysis. J ISAKOS 2016 Mar;1(2):70-81.
- 4. Hirtler L, Kainberger F, Röhrich S. The intercondylar fossa-A narrative review. Clin Anat 2022 Jan;35(1):2-14.
- 5. van Eck CF, Martins CA, Vyas SM, Celentano U, van Dijk CN, Fu FH. Femoral intercondylar notch shape and dimensions in ACL-injured patients. Knee Surg Sports Traumatol Arthrosc 2010 Sep;18(9):1257-1262.
- 6. Kim SH, Lee JW, Kim MG, Kim KI, Lee SH. Radiologic findings associated with mucoid degeneration of the anterior cruciate ligament. Arch Orthop Trauma Surg 2023 Jul;143(7):4257-4265.
- 7. Raja B, Marathe N, Desai J, Dahapute A, Shah S, Chavan A. Evaluation of anatomic risk factors using magnetic resonance imaging in non-contact anterior cruciate ligament injury. J Clin Orthop Trauma 2019;10(4):710-715.
- 8. Alentorn-Geli E, Pelfort X, Mingo F, Lizano-Díez X, Leal-Blanquet J, Torres-Claramunt R, et al. An evaluation of the association between radiographic intercondylar notch narrowing and anterior cruciate ligament injury in men: the notch angle is a better parameter than notch width. Arthroscopy 2015 Oct;31(10):2004-2013.
- 9. Fernández-Jaén T, López-Alcorocho JM, Rodriguez-Iñigo E, Castellán F, Hernández JC, Guillén-García P. The importance of the intercondylar notch in anterior cruciate ligament tears. Orthop J Sports Med 2015 Aug;3(8):2325967115597882.
- 10. Ficek K, Rajca J, Cholewiński J, Racut A, Gwiazdoń P, Przednowek K, et al. Analysis of intercondylar notch size and shape in patients with cyclops syndrome after anterior cruciate ligament reconstruction. J Orthop Surg Res 2021 Sep;16(1):554.
- 11. Huang M, Li Y, Guo N, Liao C, Yu B. Relationship between intercondylar notch angle and anterior cruciate ligament injury: a magnetic resonance imaging analysis. J Int Med Res 2019 Apr;47(4):1602-1609.