Localized Persistent Pulmonary Interstitial Emphysema in a Pre-term Neonate-A Case Report
Hilal Al Mandhari,1 Masood Ahmed,1 Madhavan Nair,2 Hussein A Al-Kindy,3 Lalitha Krishnan4
Al Mandhari H, et al. OMJ. 25, (2010); doi:10.5001/omj.2010.42
ABSTRACT
Persistent pulmonary interstitial emphysema is a rare disorder of pre-terms seen even in non-ventilated neonates. The condition needs to be differentiated from other neonatal lung anomalies requiring early surgery, because there is a role for conservative management of these babies. CT scan findings are typically helpful in diagnosis.
From 1Department of Neonatal Unit, Child Health Department, Sultan Qaboos University Hospital, 2Department of Pediatric Surgery, Royal Hospital, 3Department of Pulmonology, Child Health Department, Sultan Qaboos University Hospital, 4Department of Child Health Department, Sultan Qaboos University Hospital, Oman.
Received: 15 Jan 2010
Accepted: 21 Feb 2010
Address of correspondence and reprint request to: Dr Lalitha Krishnan, Consultant, Neonatal unit, Child Health Department, Sultan Qaboos University Hospital, Muscat, Oman
E-mail: lalitha_krishnan@hotmail.com
Al Mandhari H, et al. OMJ. 25, (2010); doi:10.5001/omj.2010.42
INTRODUCTION
Pneumothorax and pulmonary interstitial emphysema (PIE) are the most common causes of air leak syndromes in the newborn period.1 They are typically described in mechanicallyventilated premature infants with respiratory distress syndrome. Localized persistent pulmonary interstitial emphysema (PPIE) is an uncommon form of interstitial emphysema with characteristic X-ray and CT findings. This is a case report of PPIE in a preterm baby who developed recurrent left-sided pneumothorax on nasal CPAP. CT scan showed multiple air-filled cysts in the left upper lobe. Lobectomy was performed, after which the baby did well.
A male baby was born to a gravida 4, para 3 mother, at 34wks
gestation by emergency lower segment cesarean section. The baby
cried immediately after birth, but developed secondary apnea
requiring bagging with a mask for approximately 30 seconds. He
was admitted to the neonatal intensive care unit with tachypnea
and recessions, for which he was started on 5 cm nasal continuous
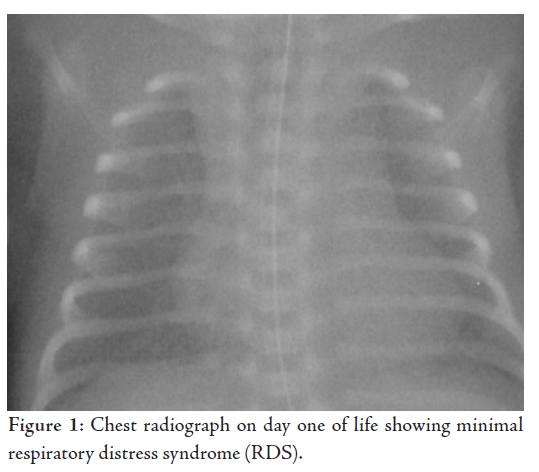
positive airway pressure (CPAP). The chest X-ray performed at 6
hrs of life was consistent with mild respiratory distress syndrome
(RDS). The baby showed clinical improvement over the next 36
hrs. At this time, the baby became more distressed and the FiO2
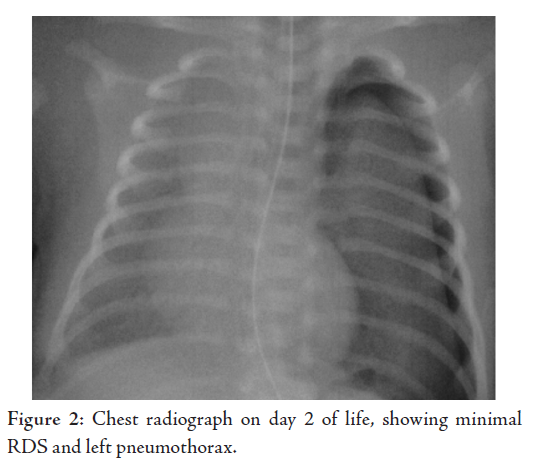
requirements increased. A repeat chest X-ray was performed,
which showed a large left pneumothorax, (Fig. 2). An intercostal
chest drainage (ICD) tube was inserted and nasal CPAP was
continued. The next day, in spite of a functioning ICD in situ, the
baby developed sudden desaturation and bradycardia, for which
he had to be intubated and ventilated. The baby was extubated
three times over the next 7 days and had to be re-intubated each
time, ventilated with chest tube re-insertion because of recurrent
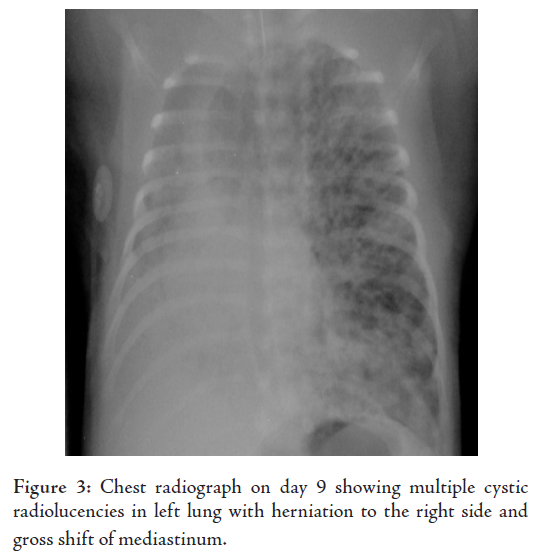
Repeated chest X-rays performed during this period showed
multiple cystic radiolucencies in the left upper lobe, with
herniation and mediastinal shift to right, (Fig. 3). A CT chest scan
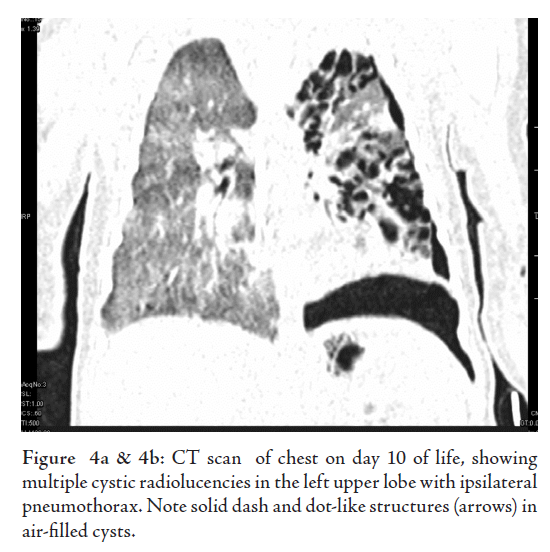
was performed, which showed multiple air-filled cysts localized in
the left upper lobe with collapse of the left lower lobe with typical
line and dot structures in air-filled cysts, (Fig. 4). Because of the
need for repeated intubation, chest drain insertion and mechanical
ventilation, surgery was then considered.
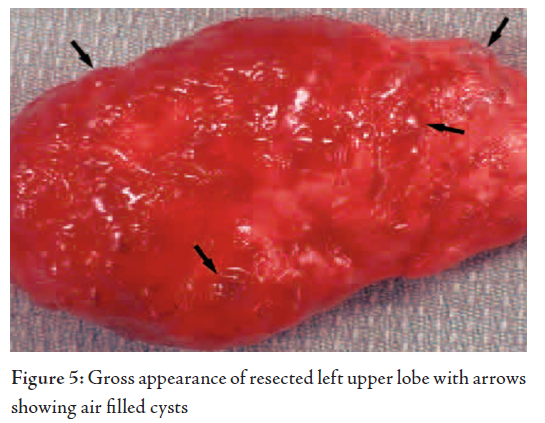
The baby underwent lobectomy of the left upper lobe which
showed multiple cysts on the surface of the lung, (Fig. 5). The
histopathology of the excised lobe showed several irregular
dilated interstitial spaces in the interlobular septae. High power
magnification showed foreign body giant cells lining these spaces,
the alveolar spaces were normal with areas of hemorrhage. Postoperatively,
the baby was extubated and the chest tube was
removed without any complications. The baby did well and was
discharged home by day 28 of life.
Pneumothorax and pulmonary interstitial emphysema (PIE) are the most common causes of air leak syndromes in the newborn period.1 During mechanical ventilation, barotrauma to the alveoli produces rupture of the alveolar space at its junction with less expandable fluid-rich perivascular connective tissue. The air leaks into the perivascular sheath and dissects it, giving rise to pulmonary interstitial emphysema, pneumothorax, and pneumomediastinum.2 Pulmonary interstitial emphysema can be classified clinically as acute (<7 days duration) or persistent (PPIE). PPIE is subclassified as localized or diffuse, according to the extent of involvement.3 Clinically, acute pulmonary interstitial emphysema most commonly develops with hyaline membrane disease. Less commonly, it could develop with meconium aspiration (air trapped behind an obstruction) or pulmonary hypoplasia, requiring high ventilatory pressure. This typically lasts for a short duration. Localized PPIE however, often occurs spontaneously with no apparent lung disease or assisted ventilation. Pursnani et al. described PPIE in a term baby with no previous history of mechanical ventilation, who presented with tension pneumothorax.1 While Jabra et al. reported a case of localized PPIE in a preterm infant who received nasal CPAP at 4-6cm of water for management of RDS.3 This baby did well initially and was in room air by day 13 of life, although his chest X-rays began to show cystic lesions by day 3 of life. The lesions were progressively increasing in size until the baby became symptomatic by day 14, after which he was operated. Bas et al. also reported a case of localized PPIE in a preterm infant who initially received nasal CPAP for 3 days, and later presented at 24 days of life with respiratory distress.4 The chest X-ray and CT chest scan showed cystic lung lesions in the left upper lobe. Studies have suggested that PPIE has typical chest X-ray and CT findings. On CT, PPIE is associated with solid linear or dot-like structures within air filled cysts, as was demonstrated in this report.3 This has been considered to be a specific sign of PPIE, which was presented in 82% of cases in one series.5 This occurs because of gas in the pulmonary interstitial space surrounding the bronchovascular bundles. The vessels appear as lines or dots depending on the orientation of the vessel in relation to the plane of the CT image. The other local lung lesions that have to be differentiated are congenital cystadenomatoid malformation, congenital lobar emphysema, bronchogenic cysts and cystic lymphangioma. This is important because early definitive surgical treatment may have to be planned for these conditions. Conservative management for PPIE has been recommended, which includes high frequency ventilation, selective intubation of contralateral bronchus and decubitus positioning of the baby.4,5,6 In a series of 17 patients, all were initially treated conservatively.5 Nine eventually underwent surgical resection, indications for surgery included unmanageable respiratory distress caused by mass effect or the increasing size of lesions over a prolonged period in symptomatic patients. Among the 10 patients who underwent nonsurgical treatment for at least 1 year, lesions as well as symptoms resolved in four patients, and lesions decreased in size in three patients whose symptoms resolved. Lesions enlarged in three patients, two eventually underwent resection, and the third patient was treated without surgery because the patient?s symptoms were stable and the lesions were bilateral. In this study, surgery was planned because there was recurrent tension pneumothorax requiring ICD.
CONCLUSIONIn conclusion, PPIE is a rare condition and may be seen in preterms who receive no ventilatory support or were managed only with nasal CPAP for RDS. The condition exhibits typical chest CT findings which help in differentiating it from other lung conditions such as congenital lobar emphysema or congenital cystadenomatoid malformation which requires urgent surgery. There is good scope for conservative management although eventually, approximately half the patients end up requiring surgical resection.
The authors reported no conflict of interest and no funding was received on this work.
-
Pursnani SK, Amodio JB, Guo H, Greco MA, Nadler EP. Localized persistent interstitial pulmonary emphysema presenting as a spontaneous tension pneumothorax in a full term infant. Pediatr Surg Int. 2006; 22(7):613- 616.
-
Oh MH, Kim MY, Shim WS, Oh SS, Shin BK, Cho SJ, et al. A case of localized persistent interstitial pulmonary emphysema. J Korean Med Sci. 2001; 16(2):225-228.
-
Jabra AA, Fishman EK, Shehata BM, Perlman EJ. Localized persistent pulmonary interstitial emphysema: CT findings with radiographicpathologic correlation. AJR Am J Roentgenol. 1997; 169(5):1381-1384.
-
Bas AY, Okumus N, Demirel N, Zenciroglu A. Persistent pulmonary interstitial emphysema in a preterm infant. Indian Pediatr. 2008; 45(9):775- 777.
-
Donnelly LF, Lucaya J, Ozelame V, Frush DP, Strouse PJ, Sumner TE, et al. CT findings and temporal course of persistent pulmonary interstitial emphysema in neonates: a multiinstitutional study. AJR Am J Roentgenol. 2003; 180(4):1129-1133.
-
Cohen RS, Smith DW, Stevenson DK, Moskowitz PS, Graham CB. Lateral decubitus position as therapy for persistent focal pulmonary interstitial emphysema in neonates: a preliminary report. J Pediatr. 1984; 104(3):441- 443.