Epidemiological Characteristics of Corneal Ulcers in South Sharqiya Region
Keshav BR, Zacheria G., Ideculla T., Bhat V., Joseph M.
ABSTRACT
Aim: To understand the epidemiology, predisposing factors, etiology and the outcome of management of corneal ulcers in South Sharqiya region of Oman.
Methods: 188 patients who presented to us in eye Ophthalmology Department of Sur regional hospital with corneal ulcers were analyzed retrospectively. The historical aspects including the systemic and local predisposing factors, clinical picture of the ulcer which was noted on slit lamp at the time of presentation, results of culture for which material was taken by scraping of the ulcer, and its sensitivity pattern, type of management, and its outcome, were noted and the results were interpreted.
Results: 60.83% were males above the age of 60 years. Severe ulcers were seen in 36.17% of cases. 43.18% of cases showed positive culture of which 88.2% were bacteria and rest were fungal isolates. Of the bacteria 53.84% were pseudomonas, and 20% staphylococcus. 83.5% were put on fortified gentamycin and 68.61% were on cefuroxime in the initial dual therapy. 37.23% were on ciprofloxacin one time or another during the course of the ulcer. 69.14% of cases recovered fully and 9.57% improved. 54.25% needed hospitalization for less than 1 week and 34% for less than 2 weeks. 58.76% of cases recovered in less than 3 weeks. As local predisposing factors 45 cases (24%) were post surgery, and 29 cases (15.4 %) were having CDK (climatic droplet keratopathy). Diabetes was seen in 8.5% of cases.
Conclusion: Corneal ulcer was seen predominantly in males above the age of 60 years, pseudomonas being the main etiological organism. Dual therapy was the commonest empirical therapy. No major systemic risk factor was identified. Post surgical and CDK were the predominant local risk factors.
Key words: corneal ulcer; pseudomonas; dual therapy.
Submitted: 3 May 2007
Reviewed: 11 July 2007
Accepted: 28 Oct 2007
From the Department of Ophthalmology, Sur Hospital
Address correspondence and reprint request to: Dr. Keshav, Head of Department of Ophthalmology, Sur hospital, South Sharqiya Region, Sultanate of Oman
P.O. Box 823, P.C. 411
E-mail: keshavraj_2000@yahoo.com
INTRODUCTION
Corneal ulcer is a sight threatening disorder presenting in all age groups and either sex world wide. It may resolve without any sequelae, progress to perforation and its resultant consequences, or leave behind an opacity which if central may lead to loss of vision. In Oman, corneal opacity is the leading cause of blindness followed by cataract.1 The various risk factors for corneal ulcers and its mode of presentations are rife in literature but they vary from region to region as it depends on the culture, socioeconomic status, occupation, habits, etc, of a particular place/region. The antibiotic sensitivity also varies from region to region. Due to the above stated reasons this study was taken up to evaluate the various risk factors, age and sex predilections, the type of microbes causing the ulcers and the type of antibiotics the organisms are sensitive to so that a systematic approach may be adopted in preventing and treating this sight threatening disorder.
The aim of the study is to study the epidemiology of corneal ulcer in South Sharqiya region, the various risk factors and predisposing factors in corneal ulcers, and the bacterial/fungal spectrum causing the ulcers and to determine the best possible empirical therapy and specific therapy for these ulcers please the literature.
METHODS
Patients: One hundred and eighty eight patients treated for corneal ulcers in Sur regional hospital between 14th October 2000 and 19 Nov 2006 were included in the study. The catchment area has population of 1: 70000. Almost all cases were advised admission. Corneal ulcer was defined as loss of corneal epithelium with underlying infiltration and suppuration with surrounding inflammation with/without hypopyon.2 In all these patients, symptoms, duration of ulcer, relevant systemic conditions like diabetes, immunosuppression, prolonged hospitalization if any were asked and recorded.
Clinical procedures: In most of the cases visual acuity where possible was measured and a detailed slit lamp examination of the anterior segment was performed wherever possible noting the size of ulcer, depth and extent of infiltrations, presence/absence of hypopyon, scleral extension, corneal thinning and so on and the ulcer was graded as mild, moderate or severe as per the Jones guidelines.3 Local eye conditions predisposing to corneal ulceration like lagophthalmos, dacryocystitis, trichiasis, surgery and corneal opacity/degeneration were noted. Materials were taken from the ulcers with a 23g needle/scalpel from the base and edges of the ulcer and inoculated by linear streaking in blood, chocolate and mcconkeys media and sent to the lab for culture sensitivity. Bacterial cultures were reported after 48 hrs of incubation. In almost all cases, admission was ensured and started on dual (fortified gentamycin+fortified cefuroxime)/monotherapy (ofloxocin) empirically. When a fungal etiology was suspected or in cases not responding to antibacterial treatment, material was taken from such ulcers for KOH smear and inoculation in Sabaorauds medium.
Our earlier protocol was to go by the clinical picture and if not suggestive of fungal we would not send the sample in sabaurauds in the first instance. Another reason being that saborauds medium was not routinely available when these samples were sent.
Progress of the ulcer was noted every day, when in the hospital by measuring the size of the ulcer, observing the hypopyon if present, infiltrations and patient’s symptoms. Patients were discharged usually when the ulcer showed signs of regression and if the patient seemed compliant to therapy. The size of the ulcer asvisual acuity is only affected if the ulcer is central.
Laboratory: Bacterial growth in culture media was considered significant if it was observed in two solid phase media or confluent growth in one media. Fungal isolation in SDA (sabaurauds dextrose agar) or observation of hyphal filaments in KOH smear was considered sufficient for diagnosis.
RESULTS
Of the 188 patients, 121 (64.36%) were males and 67 (35.73%) were females. 24 patients (12.76%) were <30 years of age, 43 (22.87%) were 30-60 years of age and 121 (64.36%) were >60 years of age (Figure 1). Thus males and patients above the age of 60 years showed greater frequency of corneal ulcer.
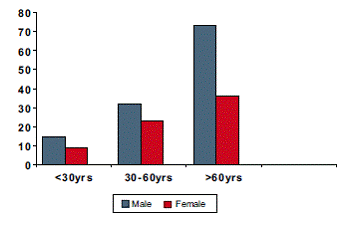
Figure 1: Shows proportion of males and females among
the various age groups of patients
With regards to severity of ulcers, the ulcers were graded as per Jones guidelines and we found that 65 cases (34.57%) had mild ulcers, 55 cases (29.25%) had moderate ulcers and 68 patients (36.17%) had severe ulcers. (Figure 2)
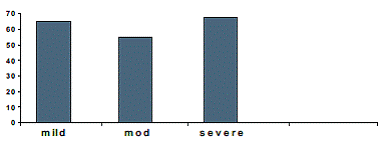
Figure 2: Shows the various grades of severity of corneal ulcers
in the studied subjects
Thus severe ulcers were marginally in higher numbers as compared to other types of ulcers.100 patients (53.19%) showed hypopyon while the rest had no hypopyon showing almost the same frequency. Most of the patients in whom visual acuity was elicited showed a vision of < 3/60 (120 patients-65%), 43 patients (22.87%) were blind and 22 patients (11.89%) had a vision of > 3/60. (Table 1)
Table 1: Shows the Visual status of patients in the study
NPL |
<3/60 |
>3/60 |
43 |
120 |
22 |
23.24% |
64.86% |
11.89% |
NPL: No Perception of Light |
||
When microbiological isolation was evaluated it was found that in 76 patients (43.18%) bacteria/fungi was isolated where material was sent for culture/sensitivity and in 100 patients (56.81%) no isolate was seen.9 Patients (5.1%) showed fungal isolates. In 12 patients scraping could not be done. (Figure 3)
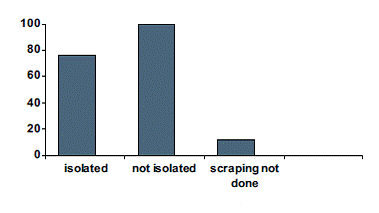
Figure 3: Shows the proportions of patients with positive
and negative microbial isolation on culture
Thus 43.18% of patients in the study showed either bacteria/fungus in culture. Among the isolates, 9 cases (11.84%) were fungi and the rest (88.26%) were bacteria. Of the bacterial isolates, pseudomonas was found in 35 cases (53.84%), staphylococci was found in 13 cases(20%), streptococcus pneumonia was found in 12 cases (18.46%), streptococci was found in 2 cases (3%) and klebsiella was found in 5 patients (7.69%). (Figure 4)
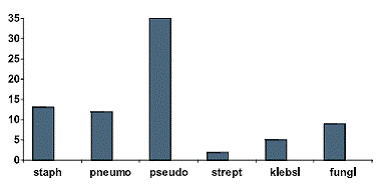
Figure 4: Shows the proportion of patients with specific
microbial isolates in positive cultures
Thus in over half the cases with bacterial isolates, pseudomonas was seen (53.84%).
In so far as treatment is concerned, almost all patients suspected to be bacterial were started on dual treatment of fortified gentamycin (14mgm/ml) and cefuroxime (50mgm/ml) as empirical therapy. 157 patients (83.5%) were given fortified gentamycin and 129 patients (68.61%) were given cefuroxime. 70 patients (37.23%)were given T. Ciprofloxacin, 21 patients (11.17%) were administered ofloxacin eye drops as initial line of therapy. 51 patients (27.12%) were covered with fucidic acid ointment at night. 22 patients (11.70%) were changed to ceftazidime (50mgm/ml) based on the c/s report when the ulcer was not responding. 16 patients (8.51%) got ceftriaxone drops (50mgm/ml). Cephradine drops (4 patients) and vancomycin drops (7 patients) were administered in a small proportion of patients. Ketoconazole drops 2 mgm/ml formed by dissolving 200 mgm tab in artificial tears was given to 20 patients (10.63%) who were suspected or proven to have fungal ulcers. Amphotericin drops were started in 6 patients (3.19%) with fungal ulcers. (Figure 5)
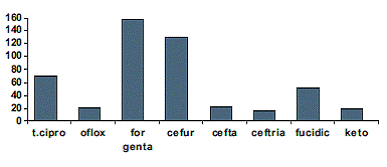
Figure 5: Shows the various antibiotics that the study patients
were put on for treatment of corneal ulcer
When the response to treatment were analyzed it was seen that around 130 (69.14%) patients recovered, 18 (9.57%) patients showed signs of regression but failed to keep up the appointment to assess the course of the ulcer, 10 (5.31%) patients the ulcer remained stationary and left seeking advice elsewhere, 17 (9%) patients left against medical advise and 9 cases (4.78%) worsened. (Figure 6)
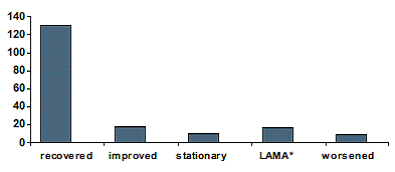
Figure 6: Shows the outcome of treatment in patients enrolled in the study
Thus a majority of patients responded to our line of management with only 9 cases showing signs of progression/worsening.
When the length of hospitalization was analyzed it was seen that 102 patients (54.25%) stayed for less than a week and 64 patients (34%) stayed for 1-2 weeks and the rest stayed for more than 2 weeks. (Table 2)
Table 2: Shows the length of hospitalization and time taken for recovery in our patients
|
Less than 1 week |
More than 1 week & less than 2 week |
More than 2 weeks & less than 3 weeks |
More than 3 weeks |
Length of stay |
102(54.25%) |
64(34%) |
13(6.9%) |
9(4.78%) |
Time for recovery |
26(19.8%) |
37(28.2%) |
14(10.68%) |
53(40.45%) |
Thus, majority (88%) of patients were discharged within 2 weeks.
With regards to the time of recovery, it was found that 26 patients (19.84%) took less than a week to recover, 37 patients (28.24%) took 1-2 weeks to recover, 14 patients (10.68%) took 2-3 weeks to recover and 53 patients (40.45%) took more than 3 weeks to recover. (Table 2) Thus, around 40% of cases required more than 3 weeks for recovery and 60% took less than 3 weeks.
Of the relevant eye conditions predisposing to c.ulcer it was found that about 45 patients (24%) had undergone intraocular surgery one time or other before the development of ulcer. 15 patients (8%) showed trichiasis, 29 patients (15.4%) showed corneal degeneration, 11 cases (5.85%) had h/o trauma, 4 patients (2.12%) gave h/o C.L.wear, 3 patients (1.59%) were on local steroids, glaucoma was present in 27 patients (14.36%) and 5 patients had corneal opacity, 2(1%) patients had proptosis and 7 patients (3.72%) had blepharitis. (Table 3)
Table 3: Shows the associated local eye conditions in the patients enrolled in the study
Proptosis |
Post-operative |
Blepharitis |
Trichiasis |
Corneal. deg |
Trauma |
CL* |
Drugs |
Glaucoma |
Corneal opacity |
02 |
45 |
7 |
15 |
29 |
11 |
4 |
3 |
27 |
5 |
1.06% |
23.93% |
3.72% |
7.97% |
15.42% |
5.85% |
2.12% |
1.59% |
1.43% |
2.65% |
*CL: Contact Lens |
|||||||||
Among the systemic diseases diabetes was noted in 16 patients (8.5%) while 1 patient was debilitated.
Of the complications perforation at the time of presentation or after starting treatment in the hospital was seen in 33 patients (17.55%), 6 patients (3.19%) developed descemetocele, 4 patients (2.12%) developed endophthalmitis and 12 (6.38%) patients had non-healing ulcers or persistent epithelial defect. (Table 4)
Table 4: Shows the proportion of patients with various complications
Perforation |
Descemetocele |
Endophthalmitis |
Recurrent/non healing |
33 |
06 |
04 |
12 |
17.5% |
3.19% |
2.12% |
6.38% |
DISCUSSION
Corneal ulceration continues to be one of the most important causes of ocular morbidity and blindness worldwide. In a national survey conducted in 1996-97 in Oman, the prevalence of blindness was 1.1% with corneal opacity amounting to 31.6% of cases of which 79% were due to nontrachomatous causes like corneal ulcer.1 This study is a retrospective analysis of data of patients who were treated for corneal ulcers in Sur Regional hospital of South sharqiya region from October 2000 to 19th November 2006. This is the first study of its kind in this region.
In this study males clearly had higher incidence of corneal ulcers (64.36%) than females. This is in conformity with several studies conducted elsewhere like the madurai study by Srinivasan et al,2 wherein the ratio of male to female was 1.6:1 and in a study by Bashir et al,4 males again predominated. This could be explained by the fact that they are more involved in outdoor occupation and hence exposed to unfavorable circumstances like exposure to UV light especially with farmers and fishermen, trauma in agriculturists and date pickers, and so on, leading to corneal ulceration. In a study by Upadhyay et al.5 males and females were found to be equally affected.
With regards to age in our study, majority (64.36%) of them were over 60 years of age. The Madurai study also concludes the same.2 In our study patients above 60 years had many predisposing factors like CDK, dryness, cataract surgery, glaucomatous patients on medications, and lid deformities due to trachomatous scarring which probably predisposed this age group to corneal ulceration more than the other age groups. In a study by Laspina et al,6 it was found that the greatest frequency was in the age group of 30-59 years, while in our study patients between 30-60 years accounted for 23% of the cases.
When the severity of ulcers at presentation was considered, it was found that sever ulcers were marginally higher (36.17%) as compared to moderate (29.25%) and mild ulcers (34.37%). Thus, corneal ulcers occurred almost at equal frequency in so far as severity was concerned.
In a study by Mcleod et al.9 it was seen that 33 ulcers (44.59%) were moderate and 41(65.41%) were severe suggesting that severe ulcers were more often seen than moderate ulcer, although the way the severity was classified was not clear. The marginal increase in severe ulcers in our study was partly due to higher incidence of pseudomonas corneal ulcers (53.84%) as compared to other types of microbes which is known to cause severe and rapidly progressive ulcer.
Where visual acuity could be recorded on presentation, it was found that around 65% of them had a visual acuity of less than 3/60. The poor VA could be due to the ulcer itself or the predisposing factors like corneal degeneration/opacity or due to cataract. 22.87% had no perception of light at presentation. No study so far has mentioned Visual acuity at presentation. The significance of this finding is difficult to find out. Patients who were blind were seen in a quarter of our patients who are likely to suffer one type of injury or the other, or may have predisposing factors like corneal degeneration/corneal opacity or corneal edema due to absolute glaucoma.
43.18% of all the cases showed either fungus/bacteria in our study while the rest showed no isolates. In 5% of cases fungus was grown in culture. In a study by Srinivasan et al.2 68.4% showed culture positive. Bashir et al.4 showed a bacterial yield of 40% almost similar to our study. fungal growth was found in 12.5% of cases in bashers study,4 and 46.8% in madurai study.2 The low yield of fungus in our cases were probably due to the fact that cases of trauma leading to corneal ulcers were small in number (5.85%) while in madurai study it was of the order of 65.4%.
Of the bacterial isolates, 53.84 % was pseudomonas. In the Madurai study,2 the most common isolate was streptococcus pneumoniae and the author has attributed it to the large numbers of chronic dacryocystitis that was seen in his study where pneumococci was the prime isolate. In our study, pneumococci constituted 18.46% of the cases. In several other studies,4, 5 pneumococci was the most common isolate. In a study by Laspina et.al,6 coagulase negative staphylococcus was the most common isolate. The reason for the variation could be explained probably due to different climatic conditions, socioeconomic standards, culture and occupation that are seen in these geographical areas. In our study no patients had dacryocystitis while cases with corneal opacities and degenerations were seen more often. In the Madurai study, pseudomonas was seen in 14.4% of isolates. Laspina et al,6 also showed 14% of the isolates to be pseudomonas. In a study by Leck et al,7 pseudomonas was found to be the prime isolate amongst the bacterial ulcers in Ghana and in South India where similar techniques for isolation was used. In the same study the prime bacteria was streptococcus species and the author has attributed it to the changes in bacterial flora within the geographical area as influenced by climate and environment.
Majority of our patients who were started on empirical therapy were on Cefuroxime drops (68.61%) and fortified gentamycin (83.5%). Other cephalosporins like ceftriaxone, ceftazidime were administered if culture/sensitivity showed them to be effective against the isolated organism and the empirical therapy was not helping. Fucidic acid ointment was administered in 27.12 % of patients to cover the sleeping time in some cases. Monotherapy with ofloxacin was started in 11.17% of cases. In a study published in ophthalmology (no author listed),8 it was found that treatment with fortified gentamycin and cefuroxime showed equally good response when compared with ofloxcin drops and suggested monotherapy is less toxic. In our study, monotherapy was less successful than dual therapy as many patients on monotherapy had to be switched over to dual therapy in the course of treatment. This probably is because of varying sensitivity patterns in the two areas tested. In a study by McLeod et al.9 dual therapy was found to be effective in treating most bacterial corneal ulcers. Gentamycin and second to third generation cephalosporin cover a broad spectrum of bacteria and thus was found to be successful as an empirical therapy. Fluoroquinolines (Oflox and Ciprofloxacin) are not so effective against streptococcal species and increasing resistance is noted of late to these antibiotics thus may not be a suitable drug to use in empirical therapy.
With the above therapy it was found that about 60% of patients required less than 3 weeks to recover while the rest took more time to recover. In one study (no authors listed),8 it was seen that 67.9% on dual therapy were cured within 14 days of treatment. The results between the two studies are nearly comparable.
Regarding length of hospitalization, it was found that 88% of the patients were discharged in less than 2 weeks of whom over 50% were discharged in 1 week indicating that patients were discharged much before their ulcers were healed thus reducing the cost of hospitalization.
Among the patients treated about 80% showed full recovery (69.14%) or improvement following the treatment while a few worsened (4.78%) and a few of them left against medical advise suggesting that our line of treatment was fairly acceptable. This is in conformity with a study by (no authors listed),8 wherein the cure occurred in more than 60% of the cases in the two groups on either dual/monotherapy.
In various studies,2, 3, 5 trauma was a major predisposing factor while in our study trauma was seen in 5.85% of patients, a striking difference. This, also, explains the low incidence of fungal ulcers (10.63%) in our study. The number of patients with h/o Contact lens(CL) was also negligible (2%), as compared to a study by Ly CN et al.10 where 36% gave h/o CL use and Keay et al.11 showed 33.7% gave h/o CL use. The low incidence in our study was due to the fact that a majority of them were over 60 years and hail from rural areas. In a study by Basak et al.12 the number of CL users were negligible (4/1198 patients) as most of his patients were farmers from rural areas. Intraocular surgery was seen in 24% of cases and this could only be a presumed risk factor as the cornea may be more prone for ulceration than normal as they were on steroids for over a month. this can predispose the cornea to invasion by bacteria/fungi due to lowering of local resistance and to some extent presence of sutures for a long time, which may accumulate mucus and predispose the cornea for ulceration. Basak et al,12 have found only a few cases that were post surgical (8 of 1198 patients). Other risk factors like trichiasis, corneal degeneration, blepharitis, and proptosis were seen in a few cases. CDK was found in 15% of cases while in madurai study,2 it was seen in 9 of the 434 patients. Climatic droplet keratopathy is presumably caused by exposure to UV light, especially people who work outdoors are more prone for it. Frequent epithelial erosions over the mulberry deposits in CDK renders the cornea more vulnerable to ulceration.
Diabetes as a predisposing factor was seen in 8.5% of cases in Madurai study,2 and a study by Basak et al.12 (7.6%) also showed a low incidence of DM among the patients with corneal ulcer.
Perforation as a complication was seen in 17% of the cases. Either they presented to us with perforation (7 of 15 cases) or they developed this after admission. The high incidence of pseudomonas ulcer in this study can explain this complication in most of the cases.
CONCLUSION
The major aetiological agent in our study was bacterial with fungal ulcers forming a small proportion. Pseudomonas species was the major bacteria.
Fungal cases were few (5%) in our study. Dual therapy with fortified gentamycin and cefuroxime drops was effective in treating a majority of corneal ulcers.
REFERENCES
-
Khandekar R, Mohammed AJ, Negrel AD, Al Riyami A. Prevalence and causes of blindness in the Sultanate of Oman: Oman eye study, BJO 2002; 86:957-962
-
Srinivasan M, Gonzales CA, George C, Cevallos V, Mascarenhas JM, Ashokan B, et al. Epidemiology and etiological diagnosis of corneal ulceration in Madurai, South India, BJO 1997; 81:965-971
-
Jones DB. Decision making in management of Microbial keratitis, Ophthalmology 1981; 88:814-819
-
Bashir G, Shah A, Thokar MA, Rashid S, Shakeel S. Bacterial and fungal profile of corneal ulcers-a prospective study. Indian Jour. of Pathology and Microbiology 2005; 48:273-277
-
Upadhyay MP, Karmacharya PC, Koirala S, Tuladhar NR, Bryan LE, Smolin G, et al. Epidemiologic characteristics, predisposing factors and etiological diagnosis of corneal ulceration in Nepal. Am J Ophthal 1991; 111:92-99
-
Laspina F, Samudio M, Cibilis D, Ta CN, Farina N, Sanabria R, et al. Graefes Epidemiological characteristics of microbiological results on patients with infectious corneal ulcers: A 13 year survey in Paraguay, Arch Clin Exp Ophthalmology 2004; 242:204-209
-
Leck AK, Thomas PA, Hagan M, Kaliamurthy J, Ackuaku E, John M, et al. Etiology of supportive corneal ulcers in Ghana and south India and epidemiology of fungal keratitis. BJO 2002; 86:1211-1215
-
(No authors listed) Ofloxacin monotherapy for the primary treatment of microbial keratitis: a double masked randomized controlled trial with conventional dual therapy. the ofloxacin study group. Ophthalmology 1997; 104:1902-1909
-
McLeod SD, Kolahdouz-Isfahani A, Rostamian K, Flowers CW, Lee PP, McDonnel PJ. The role of smears, cultures and antibiotic sensitivity testing in the management of suspected infectious keratitis. Ophthalmology 1996;103:1165-1166
-
Ly CN, Pham JN, Badenoch PR, Bell SM, Hawkins G, Rafferty DL, et al. Bacteria commonly isolated from keratitis specimens retain antibiotic susceptibility to fluoroquinolines and gentamycin plus cephalothin. Clin Experiment Ophthalmology 2006; 34:44-50
-
Keay L, Edwards K, Naduvilath T, Taylor HR, Snibson GR, Forde K, et al. Microbial keratitis predisposing factors and morbidity. Ophthalmology 2006; 113:109-116
-
Basak SK, Basak S, Mohanta A, Bhowmick A. Epidemiological and microbiological Diagnosis of suppurative Keratitis in Gangetic West Bengal, Eastern India. Indian Journal of Ophthalmology 2005; 53:17-22